Colonoscopy
On this page:
- What is colonoscopy?
- Why do doctors use colonoscopy?
- How do I prepare for a colonoscopy?
- How do doctors perform a colonoscopy?
- What should I expect after a colonoscopy?
- What are the risks of colonoscopy?
What is colonoscopy?
Colonoscopy is a procedure in which a doctor uses a flexible tube with a camera on one end, called a colonoscope or scope, to look inside your rectum and colon. The rectum and colon make up most of your large intestine.
Colonoscopy can show irritated and swollen tissue, ulcers, polyps, and cancer.
Why do doctors use colonoscopy?
A colonoscopy can help a doctor find the cause of symptoms, such as
- bleeding from your anus
- changes in your bowel movements, such as diarrhea
- pain in your abdomen, or belly
- unexplained weight loss
Doctors also use colonoscopy as a screening tool for colon polyps and colon and rectal cancer—also called colorectal cancer. Screening is testing for diseases when you have no symptoms. Screening may find diseases at an early stage, when a doctor has a better chance of curing the disease.
Screening for colorectal cancer
Your doctor will recommend screening for colorectal cancer starting at age 45 if you don’t have health problems or risk factors that make you more likely to develop colorectal cancer.1
You may be more likely to develop colorectal cancer if you1,2
- are 45 or older
- are Black
- have a personal or family history of colorectal cancer
- have a personal history of ovarian cancer, polyps, or inflammatory bowel disease, such as ulcerative colitis and Crohn’s disease
- have Lynch syndrome or another genetic disorder that increases the risk of colorectal cancer
- have obesity, smoke cigarettes, or drink alcohol
If you are more likely to develop colorectal cancer, your doctor may recommend screening at a younger age and more often.
Colonoscopy is one test used to screen for colorectal cancer. Other screening tests may include
Talk with your doctor to see what screening options are right for you.
If you are older than 75, talk with your doctor about whether you should be screened for colorectal cancer. For more information, read the current colorectal cancer screening recommendations from the U.S. Preventive Services Task Force (USPSTF).
Government health insurance plans, such as Medicare, and private insurance plans sometimes change whether and how often they pay for cancer screening tests. Check with your insurance plan to find out how often your plan will cover a screening colonoscopy.
How do I prepare for a colonoscopy?
To prepare for a colonoscopy, you will need to talk with your doctor about any health problems you have and all medicines, vitamins, and supplements you take.
You will also need to follow a special diet for a few days, clean out your bowel, and arrange for a ride home after the procedure.
Follow a special diet
A health care professional will give you written bowel prep instructions to follow at home before the procedure, so that little or no stool remains in your large intestine. A complete bowel prep lets you pass stool that is clear and liquid. Stool inside your large intestine can prevent your doctor from clearly seeing the lining.
You may need to avoid foods that have a lot of fiber—such as whole grains, raw vegetables, beans, and nuts and seeds—several days before the procedure.
You may also need to follow a clear-liquid diet for a day or more before the procedure. The written instructions you receive will include details about when to start and stop the clear-liquid diet.
Clear liquids do not contain pulp, solids, or cream. Your doctor may also recommend avoiding red- and purple-colored drinks or gelatin. In most cases, you may drink or eat the following
- fat-free bouillon or broth
- gelatin in flavors such as lemon, lime, or orange
- plain coffee or tea, without cream or milk
- sports drinks in flavors such as lemon, lime, or orange
- fruit juice with no pulp, such as apple or white grape—avoid orange juice, pineapple juice, and other cloudy juices
- water
 You may need to follow a clear-liquid diet before your colonoscopy.
You may need to follow a clear-liquid diet before your colonoscopy.
Clean out your bowel
Different bowel preps may contain different combinations of pill, liquid, or powder laxatives. Your doctor will help you find the best bowel prep for you. Some people will drink a large amount of liquid laxative over a scheduled amount of time—most often, the night before and the morning of the procedure. Your doctor may also prescribe an enema.
The bowel prep will cause diarrhea, so you should stay close to a bathroom. This part of the bowel prep can be challenging, but it is important to finish the prep completely. Call a health care professional if you have side effects that keep you from finishing the prep.
Arrange for a ride home
Before your procedure, make plans for your recovery. For safety reasons, arrange for a ride home after the procedure, as the sedatives or anesthesia need time to wear off before you can drive.
How do doctors perform a colonoscopy?
A doctor performs a colonoscopy in a hospital or an outpatient center. A colonoscopy usually takes less than one hour.3
A health care professional will place an intravenous (IV) needle in a vein in your arm or hand to give you sedatives, anesthesia, or pain medicine. This will help you not be aware or feel pain during the procedure.
During the procedure, you’ll lie on a table while the doctor inserts a colonoscope through your anus and into your rectum and colon. The scope inflates your colon with air for a better view. The camera sends a video image to a monitor, which allows the doctor to examine the lining of your colon and rectum.
The doctor may move you several times on the table to adjust the scope for better viewing. Once the scope reaches the opening to your small intestine, the doctor slowly removes the scope and examines the colon and rectum lining again.
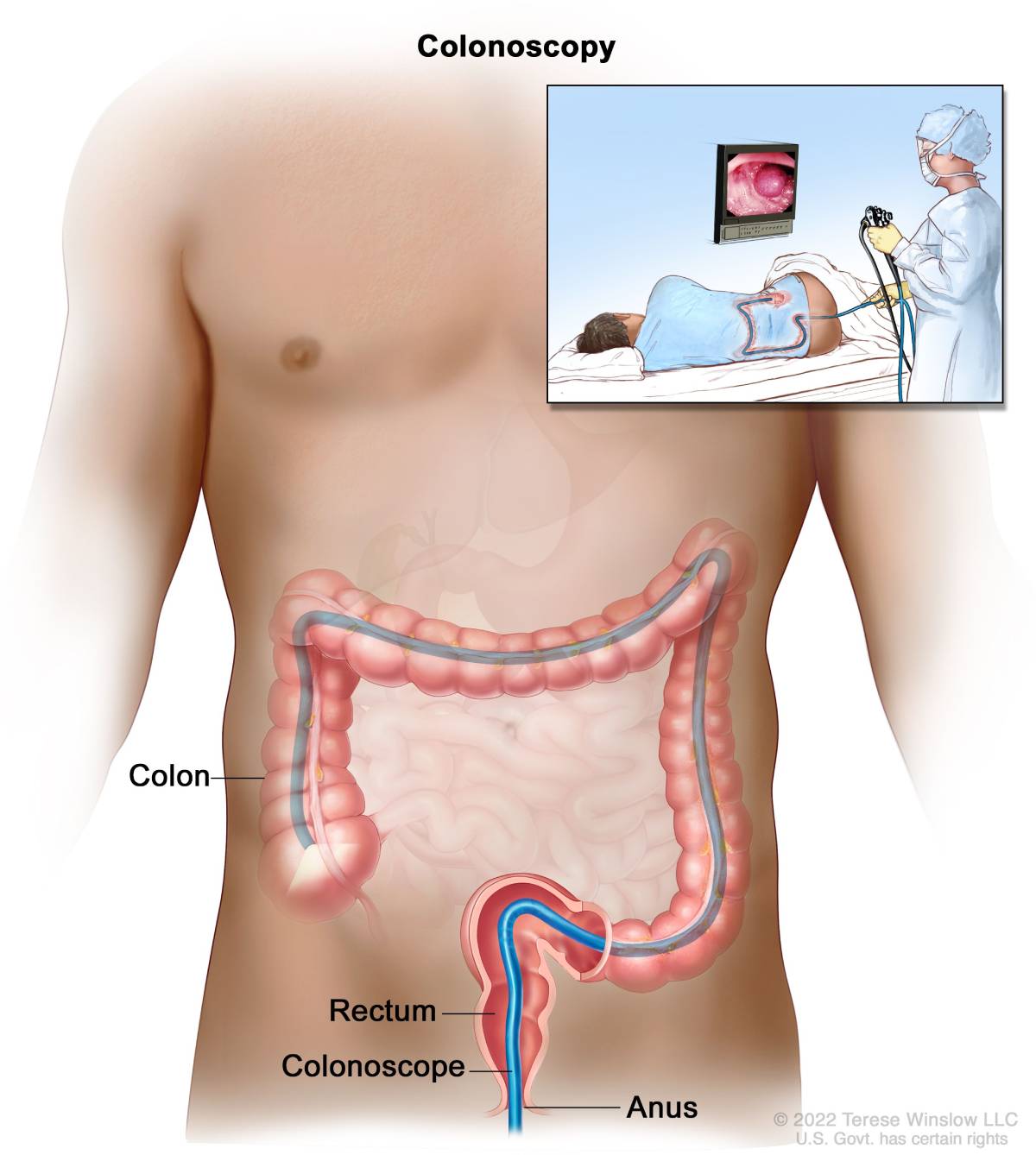 For the colonoscopy procedure, you will lie on a table while the doctor inserts a colonoscope through your anus and into your rectum and colon.
For the colonoscopy procedure, you will lie on a table while the doctor inserts a colonoscope through your anus and into your rectum and colon.
During the procedure, the doctor may remove polyps and send them to a lab for testing. You will not feel the polyp removal. Colon polyps are common in adults and are harmless in most cases. However, most colon cancers begin as a polyp, so removing polyps early may help prevent cancer.
If your doctor finds abnormal tissue, they may perform a biopsy. You won’t feel the biopsy.
What should I expect after a colonoscopy?
After a colonoscopy, the sedatives or anesthesia take time to wear off. You’ll stay at the hospital or outpatient center for about 30 to 60 minutes after the procedure.3 You may feel cramping in your abdomen or bloating during the first hour after the procedure.
After the sedatives or anesthesia wear off, your doctor may share what they found during the procedure with you or, if you choose, with a friend or family member.
You—or a friend or family member—will receive instructions on what to do after the procedure. Be sure to follow all instructions. Because you won’t be able to drive after the procedure, you’ll need your prearranged ride home.
You should expect a full recovery and return to your normal diet by the next day.
 Your doctor may share the procedure results with you after your sedatives or anesthesia wear off.
Your doctor may share the procedure results with you after your sedatives or anesthesia wear off.
If your doctor removed polyps or performed a biopsy, you may have light bleeding from your anus. This bleeding is normal.
If your doctor performed a biopsy, a pathologist will examine the biopsy tissue. Results can take a few days or longer to come back. A health care professional will call you or schedule an appointment to go over the results.
What are the risks of colonoscopy?
The risks of colonoscopy include
- bleeding
- perforation of the colon
- a reaction to the sedative, including breathing or heart problems
- severe pain in your abdomen
Bleeding and perforation are the most common complications from colonoscopy. A study of screening colonoscopies found that perforation occurs in about 3 out of every 10,000 procedures.4 Bleeding occurs in about 15 out of every 10,000 procedures.4 Most cases of bleeding and perforation occur in people who are older or who have polyps removed.
Your doctor can treat bleeding that happens during the colonoscopy right away. You may have delayed bleeding up to 2 weeks after the procedure.5 If you experience delayed bleeding, your doctor may diagnose and treat it with a second colonoscopy.
Your doctor may need to treat perforation with surgery.
References
This content is provided as a service of the National Institute of Diabetes and Digestive and Kidney Diseases
(NIDDK), part of the National Institutes of Health. NIDDK translates and disseminates research findings to increase knowledge and understanding about health and disease among patients, health professionals, and the public. Content produced by NIDDK is carefully reviewed by NIDDK scientists and other experts.
NIDDK would like to thank:
Michael B. Wallace, M.D., Mayo Clinic

