Barrett’s Esophagus
Return to Overview PageDefinition & Facts
In this section:
- What is Barrett’s esophagus?
- How common is Barrett’s esophagus?
- Who is more likely to develop Barrett’s esophagus?
- What are the complications of Barrett’s esophagus?
What is Barrett’s esophagus?
Barrett’s esophagus is a condition in which the lining of your esophagus changes. The tissue that lines your esophagus becomes more like the tissue that lines your intestine. If you have Barrett’s esophagus, you may have a higher risk of developing cancer of the esophagus.
How common is Barrett’s esophagus?
Barrett’s esophagus is more common in the United States than in other countries.
The number of people in the United States with Barrett’s esophagus has increased in recent years. Researchers estimate about 5% of adults in the United States have Barrett’s esophagus. Barrett’s esophagus affects about 1% of people worldwide.1
Who is more likely to develop Barrett’s esophagus?
You are more likely to develop Barrett’s esophagus if you
- have gastroesophageal reflux disease (GERD)
- are male
- are White
- are age 50 or older
- use tobacco
- have excess weight around your waist
- have a family history of Barrett’s esophagus or esophageal cancer
What are the complications of Barrett’s esophagus?
People with Barrett’s esophagus are more likely to develop cancer in their esophagus. Before this cancer develops, abnormal cells appear in the Barrett’s tissue, or the tissue that has changed to become more like the lining of the intestine. This condition is called dysplasia.
Doctors classify dysplasia as low grade or high grade, depending on how the cells look under a microscope.
Most people with Barrett’s esophagus do not develop cancer. People with high-grade dysplasia are more likely to develop esophageal cancer than those with low-grade dysplasia or no dysplasia.
You may have Barrett’s esophagus for many years before cancer develops.
Reference
Symptoms & Causes
What are the symptoms of Barrett’s esophagus?
Barrett’s esophagus doesn’t cause symptoms. However, many people with Barrett’s esophagus also have gastroesophageal reflux disease (GERD). GERD symptoms may include
- heartburn
- regurgitation, or stomach contents coming back up into your mouth
- chest pain
- nausea
- problems swallowing or pain while swallowing
- chronic cough or hoarseness
See your doctor if you experience trouble swallowing, weight loss without trying, signs of bleeding in your digestive tract, or persistent vomiting.
 Barrett’s esophagus doesn’t cause symptoms, but you may experience heartburn or regurgitation if you also have GERD.
Barrett’s esophagus doesn’t cause symptoms, but you may experience heartburn or regurgitation if you also have GERD.What causes Barrett’s esophagus?
Researchers don’t know the exact cause of Barrett’s esophagus.
Having GERD increases your chances of developing Barrett’s esophagus. Researchers estimate about 5% to 15% of people with GERD go on to develop Barrett’s esophagus.2
Reference
Diagnosis
Who should be tested for Barrett’s esophagus?
Your doctor may recommend testing for Barrett’s esophagus if you have weekly symptoms of gastroesophageal reflux disease (GERD) for 5 or more years and at least three other risk factors for Barrett’s esophagus.3
How do doctors diagnose Barrett’s esophagus?
Doctors most often diagnose Barrett’s esophagus with an upper gastrointestinal (GI) endoscopy and a biopsy. Your doctor may also use a pill-shaped capsule device that you swallow to test for Barrett’s esophagus.
Upper GI endoscopy and biopsy
Upper GI endoscopy is a test in which a doctor uses an endoscope to see inside your upper GI tract. The test may show changes in the lining of your esophagus.
During upper GI endoscopy, a doctor takes biopsies by passing small tweezers through the endoscope. You will not feel the biopsies. A pathologist will look at the tissue under a microscope to check for Barrett’s esophagus cells.
Barrett’s esophagus can be hard to diagnose because it doesn’t affect all the tissue in your esophagus. The doctor will take biopsy samples from multiple areas of the lining of your esophagus.3
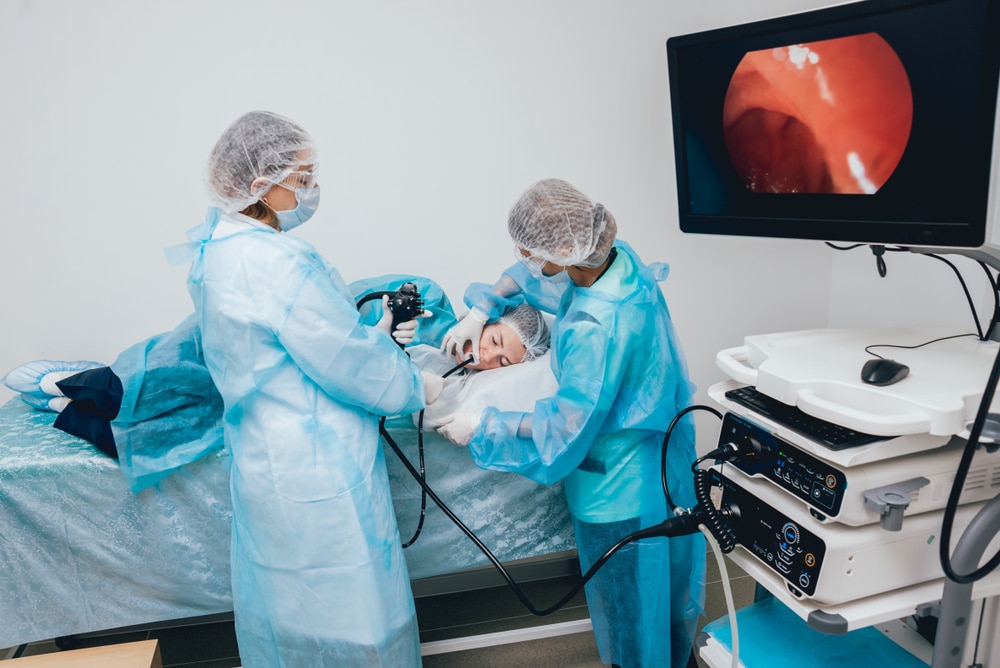 Doctors typically diagnose Barrett’s esophagus with an upper GI endoscopy and a biopsy.
Doctors typically diagnose Barrett’s esophagus with an upper GI endoscopy and a biopsy.
Repeat endoscopy
If you have Barrett’s esophagus, your doctor may repeat upper GI endoscopy and biopsy on a specific schedule to check for abnormal cells or cancer. Doctors call this approach surveillance.
Your doctor will talk with you about how often you may need a repeat endoscopy. Your doctor may recommend repeating the test more often if you have abnormal cells or cancer.
Capsule tests
To test for Barrett’s esophagus, some doctors may use a pill-shaped capsule device that you swallow. The capsule is attached to a thin string and has either a small sponge or balloon inside.
After you swallow the capsule, the sponge or balloon device expands. A health care professional then pulls the string to remove the device. On its way out, the device collects small samples of tissue from your esophagus.
The samples are tested for signs of Barrett’s esophagus.
Reference
Treatment
How do doctors treat Barrett’s esophagus?
Doctors may use medicines, endoscopy, or possibly surgery to treat Barrett’s esophagus. Talk with your doctor about which treatments are right for you.
Medicines
If you have Barrett’s esophagus and gastroesophageal reflux disease (GERD), your doctor may suggest proton pump inhibitors (PPIs). PPIs are medicines that lower the amount of acid your stomach makes. These medicines can prevent further damage to your esophagus and, in some cases, heal existing damage. Some studies have shown that PPIs may lower your chances of developing high-grade dysplasia and esophageal cancer.4 You can buy PPIs over the counter, or your doctor can prescribe one.
PPIs are generally safe and effective. Experts are still studying the effects of taking PPIs for a long period of time or in high doses.5,6 Talk with your doctor about the risks and benefits of taking PPIs.
 Your doctor may suggest PPIs to prevent further damage to your esophagus.
Your doctor may suggest PPIs to prevent further damage to your esophagus.
Endoscopy
Some doctors may treat Barrett’s esophagus during an upper gastrointestinal (GI) endoscopy. During endoscopy, doctors may
- use heat to get rid of abnormal cells in your esophagus, a treatment called radiofrequency ablation
- use cold liquid nitrogen to get rid of abnormal cells in your esophagus, a treatment called cryotherapy
- cut off and remove the Barrett’s tissue, a treatment called endoscopic mucosal resection
Surgery
Your doctor may recommend a surgery called esophagectomy to treat Barrett’s esophagus. During esophagectomy, doctors remove the affected sections of your esophagus. If a large part of your esophagus is removed, the surgeon may reshape your stomach to reconnect it to the rest of your esophagus. Surgery is less common than other ways to treat Barrett’s esophagus and may not be an option for everyone.
How can I prevent Barrett’s esophagus?
If you have GERD, managing your symptoms can prevent further damage to your esophagus. Preventing this damage may lower your risk of developing Barrett’s esophagus. Your doctor may recommend changing your eating habits and other lifestyle changes, medicines, and possibly surgery to manage symptoms of GERD.
References
Eating, Diet, & Nutrition
How can my diet help prevent or relieve Barrett’s esophagus?
Diet and nutrition may play a role in preventing gastroesophageal reflux disease (GERD), the condition that may make you more likely to develop Barrett’s esophagus.
If you have GERD, avoiding certain foods and drinks may help reduce symptoms. If you have GERD symptoms at night or when you’re lying down, eating meals at least 3 hours before you lie down may improve symptoms.7
Foods and drinks commonly linked to GERD symptoms include
- acidic foods, such as citrus fruits and tomatoes
- alcoholic drinks
- chocolate
- coffee and other sources of caffeine
- high-fat foods
- mint
- spicy foods
If you have overweight or obesity, your doctor may suggest you reach and maintain a healthy weight to help reduce GERD symptoms.
Reference
Clinical Trials
The NIDDK conducts and supports clinical trials in many diseases and conditions, including digestive diseases. The trials look to find new ways to prevent, detect, or treat disease and improve quality of life.
What are clinical trials for Barrett’s esophagus?
Clinical trials—and other types of clinical studies—are part of medical research and involve people like you. When you volunteer to take part in a clinical study, you help doctors and researchers learn more about disease and improve health care for people in the future.
Researchers are studying many aspects of Barrett’s esophagus, such as
- improving the diagnosis of Barrett’s esophagus
- understanding the causes of Barrett’s esophagus
- preventing esophageal cancer in people with Barrett’s esophagus
Find out if clinical studies are right for you.
Watch a video of NIDDK Director Dr. Griffin P. Rodgers explaining the importance of participating in clinical trials.
What clinical studies for Barrett’s esophagus are looking for participants?
You can view a filtered list of clinical studies on Barrett’s esophagus that are federally funded, open, and recruiting at ClinicalTrials.gov. You can expand or narrow the list to include clinical studies from industry, universities, and individuals; however, the National Institutes of Health does not review these studies and cannot ensure they are safe for you. Always talk with your health care provider before you participate in a clinical study.
This content is provided as a service of the National Institute of Diabetes and Digestive and Kidney Diseases
(NIDDK), part of the National Institutes of Health. NIDDK translates and disseminates research findings to increase knowledge and understanding about health and disease among patients, health professionals, and the public. Content produced by NIDDK is carefully reviewed by NIDDK scientists and other experts.
NIDDK would like to thank:
Nicholas J. Shaheen, M.D., University of North Carolina School of Medicine

