Diagnosis of NAFLD & NASH
How do doctors diagnose NAFLD?
Doctors use your medical history, a physical exam, and tests to diagnose nonalcoholic fatty liver disease, or NAFLD (also referred to as metabolic dysfunction-associated steatotic liver disease, or MASLD).
Medical history
Your doctor will ask if you have a history of health conditions or diseases that make you more likely to develop NAFLD, such as
- overweight or obesity
- insulin resistance or type 2 diabetes
- high levels of triglycerides or abnormal levels of cholesterol in your blood
- metabolic syndrome
Your doctor will ask about diet and lifestyle factors that may make you more likely to develop NAFLD, such as a lack of physical activity, eating a diet high in sugar, or drinking sugary beverages.
Your doctor will also ask about other causes of liver disease or fat in your liver. Your doctor will ask about your alcohol intake to find out whether fat in your liver is a sign of alcohol-associated liver disease or NAFLD.
 Your doctor will ask if you have a history of health conditions that make you more likely to develop NAFLD.
Your doctor will ask if you have a history of health conditions that make you more likely to develop NAFLD.Physical exam
During a physical exam, a doctor usually examines your body and checks your weight and height to calculate your body mass index.
Your doctor will also look for signs of nonalcoholic fatty liver, or NAFL (also referred to as metabolic dysfunction-associated steatotic liver, or MASL), or nonalcoholic steatohepatitis, or NASH (also referred to as metabolic dysfunction-associated steatohepatitis, or MASH), such as
- an enlarged liver
- signs of insulin resistance, such as darkened skin patches over your knuckles, elbows, and knees
- signs of cirrhosis, such as an enlarged spleen, ascites, and muscle loss
What tests do doctors use to diagnose NAFLD?
Doctors use blood tests, imaging tests, and sometimes liver biopsy to diagnose NAFLD and to tell the difference between NAFL and NASH.
Blood tests
A health care professional may take a blood sample from you and send the sample to a lab. Your doctor may suspect you have NAFLD if your blood test shows increased levels of the liver enzymes alanine aminotransferase (ALT) and aspartate aminotransferase (AST).
Your doctor may use the results of routine blood tests to calculate special scores, such as the FIB-4 or APRI. These scores can help doctors identify or rule out advanced liver fibrosis, or scarring.
Your doctor may perform additional blood tests to find out if you have other health conditions that may increase your liver enzyme levels.
Imaging tests
Routine imaging tests can show fat in your liver. These tests can’t show inflammation or fibrosis, so your doctor can’t use these tests to find out whether you have NAFL or NASH. If you have cirrhosis, routine imaging tests may show nodules, or lumps, in your liver.
Your doctor may use the following imaging tests to help diagnose NAFLD
- ultrasound, which uses a device called a transducer that bounces safe, painless sound waves off your organs to create an image of their structure
- computed tomography (CT) scan, which uses a combination of x-rays and computer technology to create images of your liver
- magnetic resonance imaging (MRI), which uses radio waves and magnets to produce detailed images of organs and soft tissues without using x-rays
Elastography is a newer type of imaging test that can help determine if you have advanced liver fibrosis. In some cases, doctors may order elastography tests to measure the stiffness of your liver. Increased liver stiffness may be a sign of fibrosis. Commonly used types of elastography are
- vibration-controlled transient elastography, a special type of ultrasound
- sheer wave elastography, another type of ultrasound to detect increased liver stiffness
- magnetic resonance elastography, a special type of MRI to measure liver stiffness
Liver biopsy
Liver biopsy is the only test that can prove a diagnosis of NASH and show clearly how severe the disease is. Liver biopsy can show fibrosis at earlier stages than elastography can. However, doctors don’t recommend liver biopsy for everyone with suspected NAFLD. Your doctor may recommend a liver biopsy if you are more likely to have NASH with advanced fibrosis or if your other tests show signs of advanced liver disease or cirrhosis. In some cases, doctors may recommend a liver biopsy to rule out other liver diseases.
During a liver biopsy, a doctor will take small pieces of tissue from your liver. A pathologist will examine the tissue under a microscope to look for signs of damage or disease.
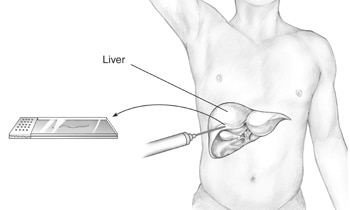 During a liver biopsy, a doctor will take a piece of tissue from your liver. A pathologist will examine the tissue under a microscope.
During a liver biopsy, a doctor will take a piece of tissue from your liver. A pathologist will examine the tissue under a microscope.
This content is provided as a service of the National Institute of Diabetes and Digestive and Kidney Diseases
(NIDDK), part of the National Institutes of Health. NIDDK translates and disseminates research findings to increase knowledge and understanding about health and disease among patients, health professionals, and the public. Content produced by NIDDK is carefully reviewed by NIDDK scientists and other experts.

