Autonomic Neuropathy
In this section:
- What is autonomic neuropathy?
- What causes autonomic neuropathy?
- What are the symptoms of autonomic neuropathy?
- How do doctors diagnose autonomic neuropathy?
- What tests do doctors use to diagnose autonomic neuropathy?
- How can I help treat autonomic neuropathy?
- How do doctors treat autonomic neuropathy?
What is autonomic neuropathy?
Autonomic neuropathy is damage to nerves that control your internal organs.
Autonomic neuropathy can lead to problems with your
- heart rate and blood pressure
- digestive system
- bladder
- sex organs
- sweat glands
- eyes
- ability to sense hypoglycemia, also called low blood glucose or low blood sugar—a condition called hypoglycemia unawareness
What causes autonomic neuropathy?
Over time, high blood glucose and high levels of fats, such as triglycerides, in the blood from diabetes can damage your nerves and the small blood vessels that nourish your nerves, leading to autonomic neuropathy.
What are the symptoms of autonomic neuropathy?
The symptoms of autonomic neuropathy depend on which of your body’s functions are affected.
Heart rate and blood pressure
Damage to the nerves that control your heart rate and blood pressure may make these nerves respond more slowly to a change in your body’s position, stress, physical activity, sleep, and breathing patterns. You may feel light-headed or faint when you stand up from lying down or sitting, or when you do a physical activity. You may have a rapid heart rate, or your heart rate may suddenly speed up or slow down. Nerve damage can also prevent you from feeling chest pain when your heart is not getting enough oxygen or when you are having a heart attack.
Digestive system
Damage to the nerves of your digestive system can cause symptoms such as the following:
- bloating, fullness, and nausea
- constipation
- diarrhea, especially at night
- diarrhea alternating with constipation
- fecal incontinence
- problems swallowing
- vomiting
Autonomic neuropathy may also cause gastroparesis. Gastroparesis is a disorder that slows or stops the movement of food from your stomach to your small intestine. Gastroparesis can keep your body from absorbing glucose and using insulin properly. These problems can make it hard to manage your blood glucose.
Bladder
Damage to the nerves of your bladder may make it hard to know when you need to urinate and when your bladder is empty. This damage can cause you to hold urine for too long, which can lead to bladder infections. You may also leak drops of urine. Leaking urine or not being able to hold urine is called urinary incontinence.
Sex organs
In men, damage to nerves in the sex organs may prevent the penis from getting firm when a man wants to have sex. This condition is called erectile dysfunction, also called ED. Men also may have problems with ejaculation.
In women, damage to the nerves in the sex organs can prevent the vagina from getting wet when a woman wants to have sex. A woman might also have less feeling around her vagina and may have trouble having an orgasm.
Sweat glands
Damage to the nerves that control your sweat glands may cause you to sweat a lot at night or while eating. Your sweat glands may not work at all, or certain parts of your body may sweat while other parts are dry. If your sweat glands do not work properly, your body may not be able to control its temperature.
Eyes
Damage to the nerves in your pupils may make them slow to respond to changes in light and darkness. Your eyes may take longer to adjust when you enter a dark room. You may have trouble seeing the lights of other cars when driving at night.
Ability to feel symptoms of hypoglycemia
Autonomic neuropathy can cause hypoglycemia unawareness, meaning that you don’t feel the symptoms of low blood glucose. Normally, early symptoms of low blood glucose can include feeling confused, dizzy, hungry, irritable, or nervous. If nerve damage keeps you from feeling these symptoms, you may not take steps to treat your low blood glucose. Without treatment, you may develop severe hypoglycemia, which can cause you to pass out. You will need help right away to deal with severe hypoglycemia.
How do doctors diagnose autonomic neuropathy?
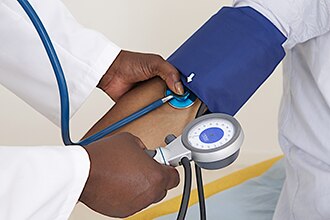
Doctors diagnose autonomic neuropathy based on your symptoms, family and medical history, a physical exam, and tests. Your doctor will check your heart rate and blood pressure and may perform additional tests to check for different types of autonomic nerve damage.
What tests do doctors use to diagnose autonomic neuropathy?
To diagnose autonomic neuropathy, your doctor may use a few tests to assess changes in your heart rate in response to simple movements such as deep breathing or standing. Your doctor may also use tests to check your sweat function to know how your nerves and sweat glands are working.
Depending on your symptoms, you doctor may also use
- tests to rule out other causes of digestive symptoms, such as constipation and diarrhea
- gastric emptying scintigraphy and gastric emptying breath tests to diagnose gastroparesis
- ultrasounds of your bladder and urinary tract to check how your bladder is working
- blood pressure checks while you are lying down and then after you stand up
How can I help treat autonomic neuropathy?
You can help treat autonomic neuropathy by managing your diabetes, which means managing your blood glucose, blood pressure, and cholesterol. Staying close to your goal numbers can keep nerve damage from getting worse.
How do doctors treat autonomic neuropathy?
Your doctor may treat the symptoms caused by autonomic nerve damage.
Heart rate and blood pressure
Your doctor will treat the symptoms of nerve damage that affect your heart rate and blood pressure. Your doctor may recommend
- getting more physical activity
- increasing salt in your diet if your blood pressure drops too low when you stand up
- increasing the amount of liquids you drink
- raising the head of your bed or wearing elastic stockings to improve blood flow
- sitting or standing slowly to prevent light-headedness or fainting
- avoiding hypoglycemia
Your doctor may also prescribe medicines that help your body retain salt, medicines to help raise your blood pressure, or medicines that raise or lower your heart rate.
Digestive system
Your doctor may recommend changes to your diet and over-the-counter or prescription medicines to treat digestive symptoms and problems such as
- constipation
- diarrhea
- fecal incontinence
- gastroesophageal reflux
- gastroparesis
Read more about these digestive symptoms and problems.
Talk with your doctor before taking any over-the-counter medicines to treat problems with digestion. Your doctor may refer you to a gastroenterologist for treatment.
Bladder
Your doctor will treat your bladder problems by focusing on your symptoms. If you have incontinence, your doctor may recommend planning regular trips to the bathroom because you may not be able to tell when your bladder is full.
Your doctor may also prescribe medicines to help with incontinence or help if you have problems completely emptying your bladder.
If you have a bladder infection, your doctor may prescribe an antibiotic and suggest drinking plenty of liquids to help prevent future infections.
Sex organs
Doctors may recommend medicines or devices to treat erectile dysfunction. Doctors may refer men to a urologist to treat sexual problems.
To treat sexual problems in women, doctors may refer women to a gynecologist. Doctors may recommend vaginal lubricants when neuropathy causes vaginal dryness.
Sweat glands
If you have too much sweating, your doctor may suggest
- avoiding too much heat or humidity
- a prescription antiperspirant or medicine to decrease sweating
- surgery to cut the nerves in the sweat glands or to remove sweat glands
Hypoglycemia unawareness
If diabetes-related nerve damage leads to hypoglycemia unawareness, you may need to check your blood glucose more often, so you know when you need to treat hypoglycemia or take steps to prevent it.
Your doctor may prescribe a continuous glucose monitor (CGM). A CGM checks your blood glucose levels at regular times throughout the day and night. CGMs can tell you if your blood glucose is falling quickly and sound an alarm if your blood glucose falls too low.
If you pass out due to severe hypoglycemia, someone will need to give you a glucagon injection and call 9-1-1. An injection of glucagon will quickly raise your blood glucose back to normal. Ask your doctor about when and how to use a glucagon emergency kit. Consider wearing a diabetes medical alert ID bracelet or pendant. If you pass out, this medical alert ID will tell other people that you have diabetes and need care right away.
This content is provided as a service of the National Institute of Diabetes and Digestive and Kidney Diseases
(NIDDK), part of the National Institutes of Health. NIDDK translates and disseminates research findings to increase knowledge and understanding about health and disease among patients, health professionals, and the public. Content produced by NIDDK is carefully reviewed by NIDDK scientists and other experts.
The NIDDK would like to thank:
Rodica Pop-Busui, M.D., Ph.D., University of Michigan

