Insulin Resistance & Prediabetes
On this page:
- What are insulin resistance and prediabetes?
- How common is prediabetes?
- Who is more likely to develop insulin resistance and prediabetes?
- What health problems can people with insulin resistance and prediabetes develop?
- What are the symptoms of insulin resistance and prediabetes?
- What causes insulin resistance and prediabetes?
- How do health care professionals diagnose insulin resistance and prediabetes?
- How can I prevent or reverse insulin resistance and prediabetes?
- Clinical Trials for Insulin Resistance and Prediabetes
What are insulin resistance and prediabetes?
Insulin resistance is a condition in which your body doesn’t respond to insulin the way it should. Insulin is a hormone made by your pancreas. Insulin resistance can lead to increased blood glucose levels, also called blood sugar levels, and weight gain. People have prediabetes if they have blood glucose levels that are higher than normal but not high enough to be diagnosed as type 2 diabetes.
If your blood glucose levels keep going up, you could develop type 2 diabetes. Type 2 diabetes can affect almost every part of your body, including your heart, eyes, kidneys, and nerves.
The good news is that many people can take steps to prevent or delay prediabetes and type 2 diabetes. If you have prediabetes or type 2 diabetes, working with your health care team to manage your prediabetes or type 2 diabetes may help you prevent other health problems.
How common is prediabetes?
In 2021, about 97.6 million people in the United States ages 18 and older had prediabetes.1 The number of adults in the United States with prediabetes, in different age groups, hasn’t changed in the last 15 years.1
People with prediabetes may be more at risk for developing type 2 diabetes. But not everyone with prediabetes develops type 2 diabetes. You can take steps to lower your risk.
Who is more likely to develop insulin resistance or prediabetes?
Certain factors can increase your chances of developing insulin resistance or prediabetes, including2
- having overweight, obesity, or a large waist size.
- being age 35 or older. Children and teens can also develop insulin resistance and prediabetes, but the risk goes up as a person gets older.
- having a family history of diabetes.
- being African American, American Indian, Asian American, Hispanic, Latino, or Pacific Islander.
- not being physically active.
- smoking, including tobacco products and e-cigarettes, or being exposed to secondhand smoke.
- having a history of gestational diabetes, a type of diabetes that develops during pregnancy, or having given birth to a baby weighing 9 pounds or more.
- having other diseases or conditions such as polycystic ovary syndrome (PCOS), Cushing’s syndrome, acromegaly, sleep apnea, or viral diseases like COVID-19.
- taking certain medicines over time, such as glucocorticoids, some antipsychotics, and some medicines for HIV.
You can’t change some of these risk factors, such as your age, your family history, or your race. However, you may be able to change some risk factors by reaching and maintaining a healthy weight, being physically active, and stopping smoking.
 You may prevent insulin resistance and prediabetes by reaching and maintaining a healthy weight and being physically active.
You may prevent insulin resistance and prediabetes by reaching and maintaining a healthy weight and being physically active.
What health problems can people with insulin resistance and prediabetes develop?
Some people with prediabetes may have changes in their blood vessels. Changes in your blood vessels can lead to some of the same health problems caused by type 2 diabetes. People with insulin resistance and prediabetes can also develop other health problems, including
- high blood pressure
- metabolic syndrome, a group of conditions—including high blood pressure and a large waist size—that increase your risk for heart disease, diabetes, and stroke
- nonalcoholic fatty liver disease, or NAFLD (also referred to as metabolic dysfunction-associated steatotic liver disease, or MASLD)
- obesity or a large waist size
- type 2 diabetes
- unhealthy levels of cholesterol and triglycerides
What are the symptoms of insulin resistance and prediabetes?
People with insulin resistance and prediabetes usually have no symptoms. Some people with prediabetes may have symptoms that are similar to symptoms of diabetes.
What causes insulin resistance and prediabetes?
Insulin resistance means that cells in your muscles, fat, and liver don’t respond well to insulin. If your cells don’t respond well to insulin, over time your pancreas may not make enough insulin to help extra glucose enter your cells. When extra glucose can’t enter your cells, you may have higher levels of glucose in your blood. When your blood glucose levels get higher than normal but not high enough to be diagnosed as diabetes, you have prediabetes.
Researchers don’t fully understand what causes insulin resistance and prediabetes. However, people with risk factors for type 2 diabetes are more likely to develop these conditions.
How do health care professionals diagnose insulin resistance and prediabetes?
Health care professionals may not test for insulin resistance. The test for insulin resistance is primarily used only for research studies.
To diagnose prediabetes, your primary health care professional may ask about your medical history and suggest blood tests. Your primary health care professional may be a doctor, physician assistant, or nurse practitioner.
Your health care professional may order tests for prediabetes if you’re age 35 or older, or if you have overweight or obesity and other risk factors for prediabetes and type 2 diabetes.
Health care professionals begin to test children who have overweight or obesity when they’re age 10 or have reached puberty.
If you have risk factors for type 2 diabetes but tests show you don’t have prediabetes, you may be retested at least every 3 years. If tests show you have prediabetes, you should be tested for type 2 diabetes every year.2
People with prediabetes have a high chance of developing type 2 diabetes within 5 to 10 years.3 You can take steps to prevent or reverse your prediabetes and prevent type 2 diabetes.
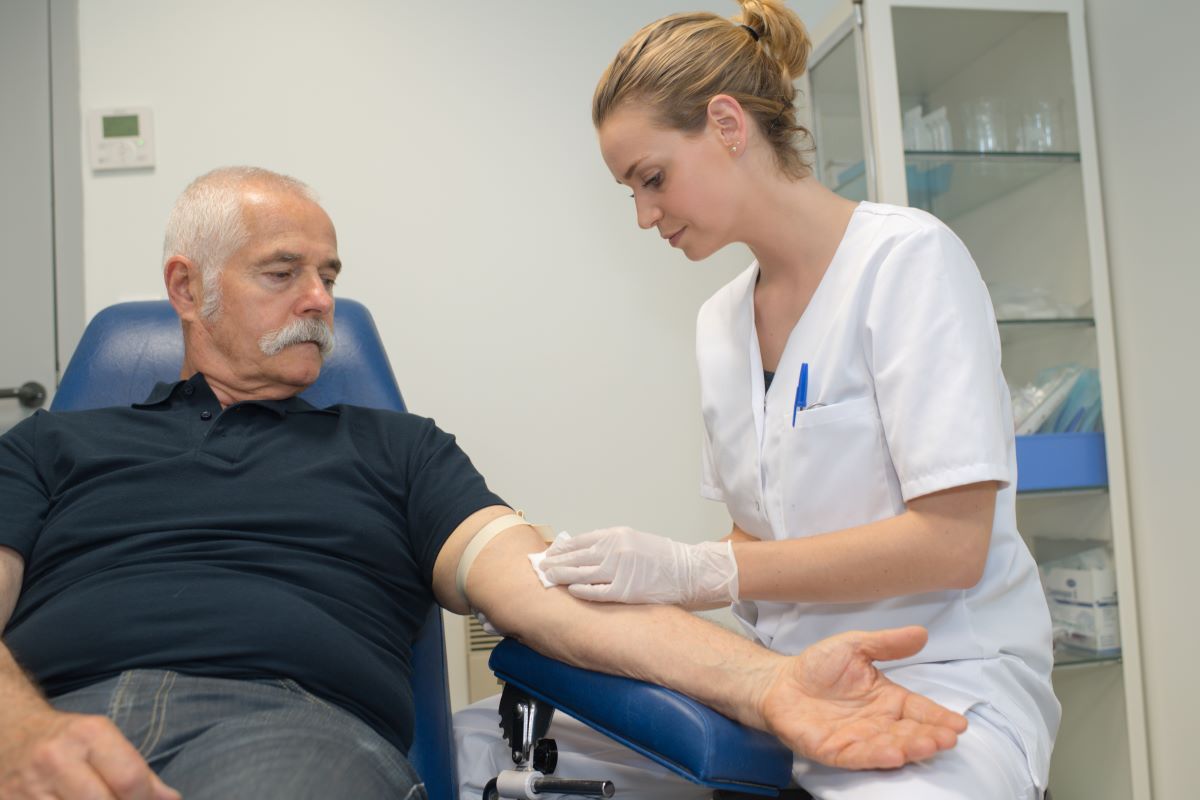 Health care professionals use blood tests to find out if you have prediabetes.
Health care professionals use blood tests to find out if you have prediabetes.
Blood tests
Health care professionals can diagnose prediabetes using blood tests that measure your blood glucose level to see if it is higher than normal. Health care professionals may use2
- the A1C test. You have prediabetes if your A1C results are between 5.7% to 6.4%.
- the fasting plasma glucose (FPG) test. You have prediabetes if your FPG results are between 100 to 125 mg/dL (milligrams per deciliter).
The FPG test shows your blood glucose level at the time of the test. The A1C test shows your average blood glucose level over the past 3 months. In people with certain health conditions, the A1C test may miss prediabetes.
Sometimes health care professionals use an oral glucose tolerance test (OGTT) to diagnose prediabetes. However, the OGTT isn’t as easy to give, takes more time, and costs more than the other tests. You have prediabetes if your OGTT results are between 140 to 199 mg/dL.2
The levels of fat in your blood may also go up when you have insulin resistance or prediabetes. Health care professionals may recommend tests for cholesterol and triglyceride levels.
How can I prevent or reverse insulin resistance and prediabetes?
To prevent or reverse insulin resistance and prediabetes, aim to live a healthy lifestyle and manage your weight. Your health care professional may also prescribe medicines to help you manage your blood glucose levels, lose weight, and prevent type 2 diabetes.
Healthy living
Healthy living may help prevent or reverse insulin resistance and prediabetes. Healthy living may also help prevent or delay the health problems related to these conditions. A healthy lifestyle may include
- consuming healthy foods and drinks
- being physically active
- managing your weight
- getting enough sleep
Making these changes can be hard. You may want to start with small changes. You can also ask for help from family, friends, and health care professionals.
Planning and tracking your progress can also help you make lifestyle changes. You may be able to take part in a lifestyle change program as part of the National Diabetes Prevention Program.
 Consuming healthy foods and drinks may help you manage your insulin resistance and prediabetes.
Consuming healthy foods and drinks may help you manage your insulin resistance and prediabetes.
Managing your weight
If you have insulin resistance or prediabetes, managing your weight can have several health benefits. Ask your health care professional or health care team if you’re at a healthy weight.
The National Institutes of Health (NIH)-funded research study, Diabetes Prevention Program (DPP), showed that for people at high risk of developing diabetes, losing 5% to 7% of their starting weight helped reduce their chance of developing the disease.4,5
If you have overweight or obesity, work with your health care team to create a plan to reach and maintain a healthy weight. Use the calculator below to find out how much 5% to 7% of your weight is and whether weight loss may help lower your diabetes risk.
Most often, health care professionals recommend lifestyle changes that may help you lose excess weight safely and keep it off. In some cases, weight-loss medicines or weight-loss surgery, also called metabolic and bariatric surgery, can be helpful.
If you’re worried about your child’s weight and they have insulin resistance or prediabetes, talk with their health care professional before your child starts a new weight-loss plan.
Medicines for insulin resistance and prediabetes
Along with healthy living and managing weight, health care professionals may also prescribe medicines such as metformin to help you manage your blood glucose levels and to prevent type 2 diabetes.
The DPP study showed that metformin could also delay type 2 diabetes. Metformin worked best for women with a history of gestational diabetes, younger adults, and people with obesity. Ask your health care professional if metformin might be right for you.
If you have health problems related to insulin resistance and prediabetes, your health care professional may prescribe other medicines, such as medicines to lower blood pressure or triglyceride levels.
Clinical Trials for Insulin Resistance and Prediabetes
NIDDK conducts and supports clinical trials in many diseases and conditions, including diabetes. The trials look to find new ways to prevent, detect, or treat disease and improve quality of life.
What are clinical trials for insulin resistance and prediabetes?
Clinical trials—and other types of clinical studies—are part of medical research and involve people like you. When you volunteer to take part in a clinical study, you help doctors and researchers learn more about disease and improve health care for people in the future.
Researchers are studying many aspects of insulin resistance and prediabetes, such as
- how diet and exercise affect insulin resistance in older adults
- how some fats can produce insulin resistance in the muscles
- how medicines, such as metformin, affect people with prediabetes and heart and blood vessel problems
Find out if clinical studies are right for you.
Watch a video of NIDDK Director Dr. Griffin P. Rodgers explaining the importance of participating in clinical trials.
What clinical studies for insulin resistance and prediabetes are looking for participants?
You can view a filtered list of clinical studies on insulin resistance and prediabetes that are federally funded, open, and recruiting at ClinicalTrials.gov. You can expand or narrow the list to include clinical studies from industry, universities, and individuals; however, the National Institutes of Health (NIH) does not review these studies and cannot ensure they are safe for you. Always talk with your primary health care professional before you participate in a clinical study.
What have we learned about insulin resistance and prediabetes from NIDDK-funded research?
NIDDK has supported many research projects to learn more about insulin resistance and prediabetes.
The Diabetes Prevention Program (DPP) and Diabetes Prevention Program Outcomes Study (DPPOS) are major studies that changed the way people approach type 2 diabetes prevention worldwide.
- The DPP study showed that people at high risk for type 2 diabetes can prevent or delay the disease with lifestyle changes that include weight loss through dietary changes and increased physical activity. The study also found that taking metformin, a safe and effective generic medicine used to treat type 2 diabetes, also prevents the disease, although to a lesser degree.
- The DPPOS continues to follow DPP participants to see if lifestyle changes or taking metformin continue to prevent or delay type 2 diabetes over time. To date, the DPPOS has shown that people can prevent or delay type 2 diabetes for at least 15 years with lifestyle changes or metformin.
References
This content is provided as a service of the National Institute of Diabetes and Digestive and Kidney Diseases
(NIDDK), part of the National Institutes of Health. NIDDK translates and disseminates research findings to increase knowledge and understanding about health and disease among patients, health professionals, and the public. Content produced by NIDDK is carefully reviewed by NIDDK scientists and other experts.
NIDDK would like to thank:
Rita Basu, M.D., University of Alabama at Birmingham

