Nephrotic Syndrome in Adults
On this page:
- What is nephrotic syndrome?
- How common is nephrotic syndrome?
- Who is more likely to develop nephrotic syndrome?
- What are the complications of having nephrotic syndrome?
- What are the symptoms of nephrotic syndrome?
- What causes nephrotic syndrome?
- How do health care professionals diagnose nephrotic syndrome?
- How do health care professionals treat nephrotic syndrome?
- How does eating, diet, and nutrition affect nephrotic syndrome?
- Clinical Trials for Nephrotic Syndrome
What is nephrotic syndrome?
Nephrotic syndrome is a group of symptoms that indicate your kidneys are not working properly. These symptoms include
- too much protein in your urine, called proteinuria
- low levels of a protein called albumin in your blood, called hypoalbuminemia
- swelling in parts of your body, called edema
- high levels of cholesterol and other lipids (fats) in your blood, called hyperlipidemia
Your kidneys are made up of about a million filtering units called nephrons. Each nephron includes a filter, called the glomerulus, and a tubule. The glomerulus filters your blood, and the tubule returns needed substances to your blood and removes wastes and extra water, which become urine. Nephrotic syndrome usually happens when the glomeruli are inflamed, allowing too much protein to leak from your blood into your urine.
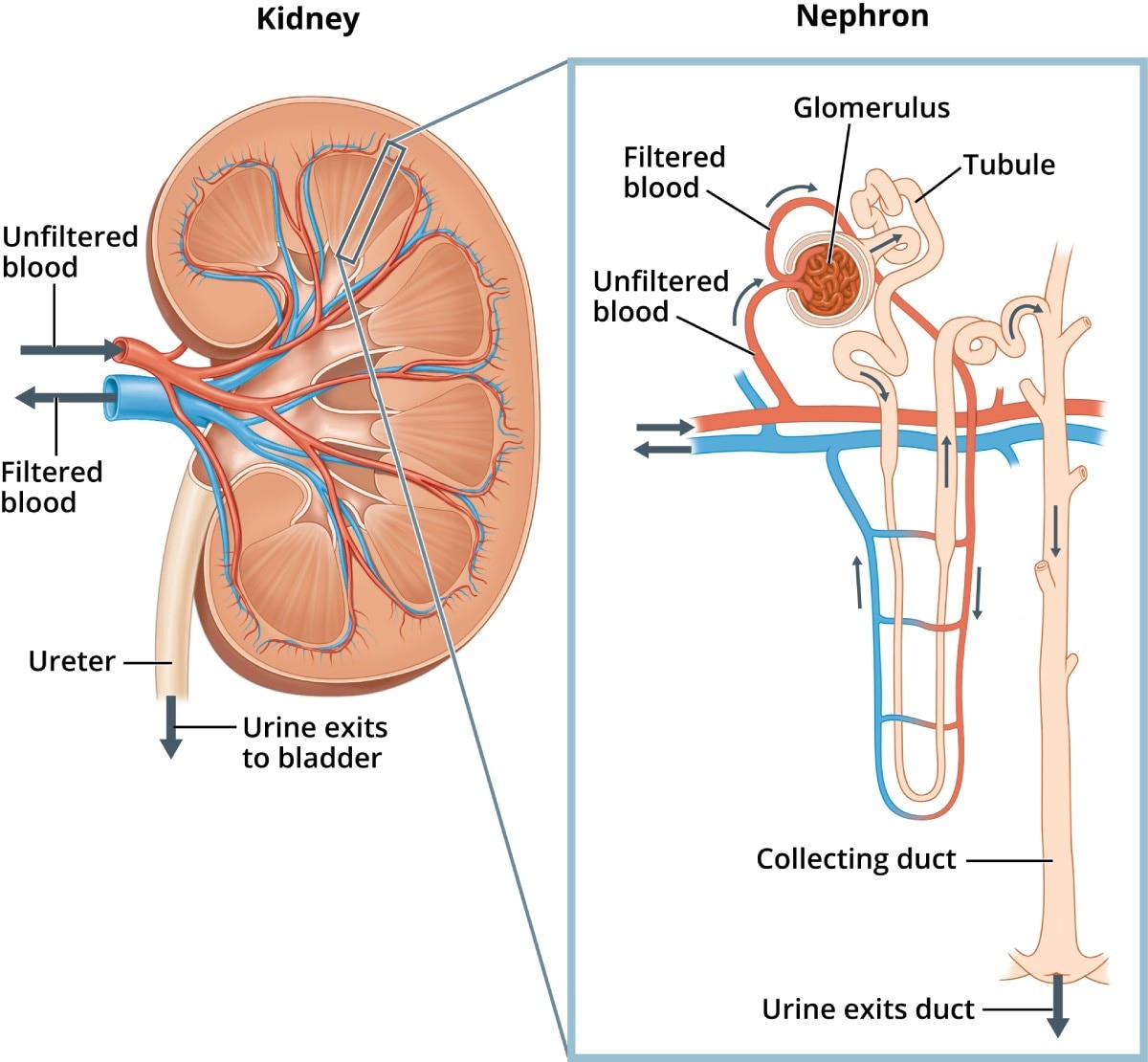 As blood passes through healthy kidneys, the glomeruli filter out waste products and allow the blood to keep the cells and proteins the body needs.
As blood passes through healthy kidneys, the glomeruli filter out waste products and allow the blood to keep the cells and proteins the body needs.How common is nephrotic syndrome?
Nephrotic syndrome is a combination of symptoms that can occur due to different causes. Among adults, the syndrome is most often caused by rare kidney diseases.
Who is more likely to develop nephrotic syndrome?
Nephrotic syndrome can affect children and adults of all ages.1
What are the complications of having nephrotic syndrome?
Nephrotic syndrome can lead to serious complications, including2
- blood clots that can lead to thrombosis
- higher risk of infection caused by the loss of immunoglobulins, proteins in your blood that help fight viruses and bacteria
- high blood pressure, also called hypertension
- brief or long-lasting kidney problems, including chronic kidney disease and kidney failure
What are the symptoms of nephrotic syndrome?
Symptoms of nephrotic syndrome can include3
- puffy eyelids and swelling in the legs, ankles, feet, lower abdomen, or other parts of your body
- foamy urine
- weight gain due to retaining too much fluid
- tiredness
- loss of appetite
What causes nephrotic syndrome?
Many disorders can cause nephrotic syndrome, including diseases that affect only the kidneys and diseases that affect many parts of the body, such as diabetes and lupus.
Kidney diseases
Diseases that affect only the kidneys and lead to nephrotic syndrome are called primary causes of nephrotic syndrome. The most common primary causes of nephrotic syndrome are3
- Focal segmental glomerulosclerosis (FSGS). This disease affects the kidney’s glomeruli, causing some of these filters to become scarred. FSGS is the most common cause of nephrotic syndrome in Black adults.
- Membranous nephropathy. This disease causes protein to build up in a part of the kidney called the glomerular basement membrane. It is the most common cause of nephrotic syndrome in white adults.
- Minimal change disease. Also called nil disease, this disease is the main cause of nephrotic syndrome in children. Among adults, nephrotic syndrome is more common in older age.
Other causes
Other causes of nephrotic syndrome, also called secondary causes, include3
- diabetes
- lupus
- amyloidosis
- infections, such as HIV/AIDS, hepatitis B, and hepatitis C
- some allergic reactions
- some medicines, such as nonsteroidal anti-inflammatory drugs
- genetic disorders that affect the kidneys
How do health care professionals diagnose nephrotic syndrome?
Your health care professional can diagnose nephrotic syndrome through urine tests. The urine tests show if you are losing too much protein in your urine.
Tests for diagnosing nephrotic syndrome
Urine dipstick test. This simple test checks for albumin in your urine. Having albumin in the urine is called albuminuria. You collect the urine sample in a container during a visit to a health care professional’s office or lab. A health care professional places a strip of chemically treated paper, called a dipstick, into the urine for the test. The dipstick changes color if albumin is present in the urine.
To confirm the diagnosis of nephrotic syndrome, your health care professional may order one of these two urine tests
- 24-hour urine collection. For this test, you will need to collect urine samples over 24 hours. Your health care professional will then send the samples to a lab for analysis.
- Urine albumin-to-creatinine ratio (UACR). The UACR test uses a single urine sample to estimate the amount of albumin lost in 24 hours. The test measures both albumin and creatinine, a waste product of normal muscle breakdown.
Your health care professional may also order blood tests to check for low levels of protein in your blood and other problems linked to nephrotic syndrome.
Tests for identifying the cause
Once nephrotic syndrome has been diagnosed, your health care professional will use tests to identify what caused it and check your kidney function. Tests for finding the cause of nephrotic syndrome can include3
- blood tests
- imaging tests, such as a kidney ultrasound
- kidney biopsy
How do health care professionals treat nephrotic syndrome?
Treating symptoms and complications
Treatment varies according to symptoms, causes, and the extent of kidney damage. Symptoms of nephrotic syndrome are most often treated with these medicines3
- an angiotensin-converting enzyme (ACE) inhibitor or an angiotensin II receptor blocker (ARB). ACEs and ARBs can help reduce protein loss and also lower blood pressure, which is often high in people with nephrotic syndrome.
- a diuretic (water pill), which reduces swelling by helping the kidneys remove fluid from the blood.
In some cases, your health care professional may also prescribe medicines that lower cholesterol, called statins. Blood thinners may also be used, but usually only if you develop a blood clot.
People with nephrotic syndrome should receive the pneumococcal vaccine, along with yearly flu shots, to prevent viral and bacterial infections.
Treating underlying causes
Other treatments vary, depending on underlying causes. In some cases, you may need to take medicines that suppress your immune system. For more on how health care professionals treat the underlying causes of nephrotic syndrome, see the NIDDK health topic Glomerular Diseases.
Once the cause has been treated, nephrotic syndrome may go away and kidney function returns to normal. Some patients may experience periods of remission followed by times when symptoms reappear. In some cases, nephrotic syndrome may lead to kidney failure.
How does eating, diet, and nutrition affect nephrotic syndrome?
Eating, diet, and nutrition have not been shown to play a role in causing or preventing nephrotic syndrome. However, if you have developed nephrotic syndrome, your health care professional may recommend that you
- limit intake of sodium (salt) and fluids to help control swelling
- reduce the amount of fat and cholesterol in your diet to help control your blood cholesterol levels
Clinical Trials for Nephrotic Syndrome
The NIDDK conducts and supports clinical trials in many diseases and conditions, including kidney diseases. The trials look to find new ways to prevent, detect, or treat disease and improve quality of life.
What are clinical trials for nephrotic syndrome?
Clinical trials—and other types of clinical studies—are part of medical research and involve people like you. When you volunteer to take part in a clinical study, you help doctors and researchers learn more about disease and improve health care for people in the future.
Researchers are studying many aspects of nephrotic syndrome, such as
- the kidney diseases that can lead to nephrotic syndrome, including genes that may cause these diseases
- quality of life among people with nephrotic syndrome
- how to best treat nephrotic syndrome
Find out if clinical studies are right for you.
Watch a video of NIDDK Director Dr. Griffin P. Rodgers explaining the importance of participating in clinical trials.
What clinical studies for nephrotic syndrome are looking for participants?
You can view a filtered list of clinical studies on nephrotic syndrome that are federally funded, open, and recruiting at ClinicalTrials.gov. You can expand or narrow the list to include clinical studies from industry, universities, and individuals; however, the National Institutes of Health does not review these studies and cannot ensure they are safe. Always talk with your health care provider before you participate in a clinical study.
References
This content is provided as a service of the National Institute of Diabetes and Digestive and Kidney Diseases
(NIDDK), part of the National Institutes of Health. NIDDK translates and disseminates research findings to increase knowledge and understanding about health and disease among patients, health professionals, and the public. Content produced by NIDDK is carefully reviewed by NIDDK scientists and other experts.
The NIDDK would like to thank:
Andrew S. Bomback, M.D., Columbia University Irving Medical Center

